I went to graduate school at the University of Arkansas and was planning on doing cancer research; that was my focus and what I enjoyed at the time. I didn’t really know how much bench work and how little patient interaction I was going to have as a PhD. After two years in the PhD program, I dropped into the Masters program and got my Masters in Anatomy and Neurodevelopmental Sciences. After that, I went to medical school in Little Rock, Arkansas and ended up staying for residency in General Surgery.

I like a lot of different things, so I thought I’d be more into something like internal medicine as a student.
My first rotation as a third-year student was vascular surgery. The very first time I learned how to scrub, on the very first day of the surgery rotation, the attending said “Who wants to cut off someone’s leg?”. I said “Uh, sure”, so we did a below the knee amputation with the vascular fellow. I got to be really hands-on and I loved doing that.
During that rotation, I got to do multiple different operations within that same kind of setting where I worked with the fellow while the attending
watches.
It wasn’t really until I switched to my next rotation in pediatrics that I really missed the operating room. I wanted to be able to make changes and see an acute change in somebody’s course. When I went to my neurosurgery rotation and I got back in the operating room I thought “I need to do something surgical. Now, what would that be?”
In residency, I was planning on doing vascular surgery but I didn’t realize how much I didn’t like endovascular surgery, so I bounced around a lot with a lot of different ideas. I ended up narrowing it down to trauma, hepatobiliary, or surgical oncology. It really came back down to a lot of the critical care stuff that we do. I ultimately wanted to be more involved in a broader spectrum of care for my patients and that’s why I decided on trauma and critical care.
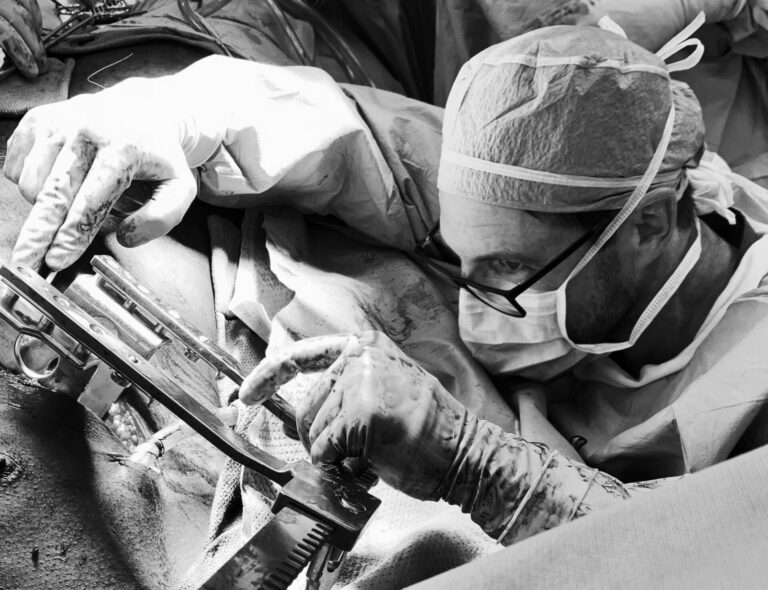
I ended up doing a fellowship at UTHSCSA and I’ve been on as faculty since 2016. I enjoy the broad spectrum of disease I see and take care of. It’s so diverse; there’s a bunch of different patient populations and different things that you see, diagnose, and treat in the ICU and Trauma bay. One night on call I may be exploring somebody’s neck, I may be exploring somebody’s chest, I may be exploring somebody’s abdomen, or I may be exploring somebody’s extremity; and that’s all in the same call. It can be very variable and I enjoy that a lot.
We didn’t have in-house faculty at my residency program, so you had to make the decision to take someone that was crashing to the operating room as a chief resident and you often had to start the case while the faculty were on their way. There were a few times that I was taking out a spleen and wondering if I was doing everything the right way before the attending even arrived. It was a daunting experience, but I think you grow up quickly when you have that responsibility on your shoulders and you have to make those decisions. While it can still be intimidating because they’re the sickest patients and they could potentially die in your hands, I feel that I got the training needed to be able to make those decisions.
I fall into a couple different niches around here.
I work with the pediatric burn program as well as serve as the Director of Emergency General Surgery. We found a real need for a pediatric burn program here because BAMC takes care of adult burn patients from all over the world but they don’t manage pediatric burns. Dr. Stewart pioneered the program to get it off the ground and Dr. Liao took over from there. As the pediatric trauma program grew larger and larger and it became more daunting to take on both that and the burn program, she handed it over to me. We see a lot of small burns like less than 5%, some medium-sized burns up to 20%, and every so often some of the larger burns up to 60-70%. So it involves a lot of initial resuscitation and then a lot of decision making when it comes to excision and grafting.
If you can sit back and identify something to learn after each experience, that will make you a better physician. We do a lot of internal review of all of our trauma patients through both a department morbidity and mortality (M&M) and a division M&M. Everyday at morning report, we discuss every patient’s case including management options and issues. There are countless times where I learn things in those situations where I’ve thought how grateful I am that we do those because we see so much. I enjoy the colleagues that I work with; they are really great and appreciative. We all work really well together and I believe that’s something that makes the job easier and more sustainable.
Trauma/Critical care has a really high burnout rate of physicians. One of the reasons for that is dealing with the situations that we deal with on a day to day basis. Having a group of people like I do that are like-minded and collegial helps there to be less burn out, less regret, less neglect; all the stuff that we do to ourselves for this job.


Story: Allison Vasak, Photographs: Supplied by Dr. Crane